Brain dead, actually, when does life end?
When your brain stops working, completely and irreversibly, you are dead; But drawing the line between life and brain death isn’t always easy. A new report attempts to clarify that distinction, perhaps helping ease the anguish of family members with a loved one whose brain has died but whose heart still beats.
Brain death has been a recognized concept in medicine for decades, but there is a lot of variation in how people define it. Demonstrating that there is some global consensus, understanding and agreement at this time will help minimize misunderstandings about what brain death is, say neurosurgeons.
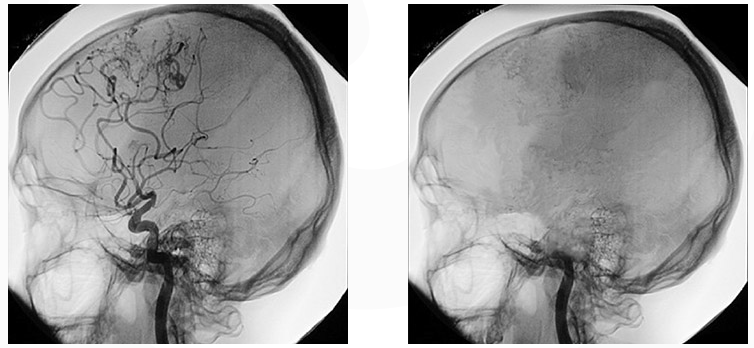
The minimum requirement to determine brain death is a good thorough clinical exam, according to a study, even before the exam is performed, doctors must verify that a person has experienced a neurological injury or condition that could cause brain death. Then doctors must look for other explanations, conditions that might mimic brain death but are actually reversible; Cooling the body, a procedure to treat heart attacks, can cause brain function to temporarily disappear, as can certain drugs, alcohol, and other toxins.
A brain death evaluation should include a series of tests for the physical responses that require a functional brain: eye movement, pain responses, and bite responses, among others. Doctors should also see if a person attempts to breathe independently, a life-sustaining process that depends on the brainstem, if none of these signs are present, a person could be considered brain dead. Additional tests, such as those that look for blood flow or electrical activity in the brain, can provide useful information.
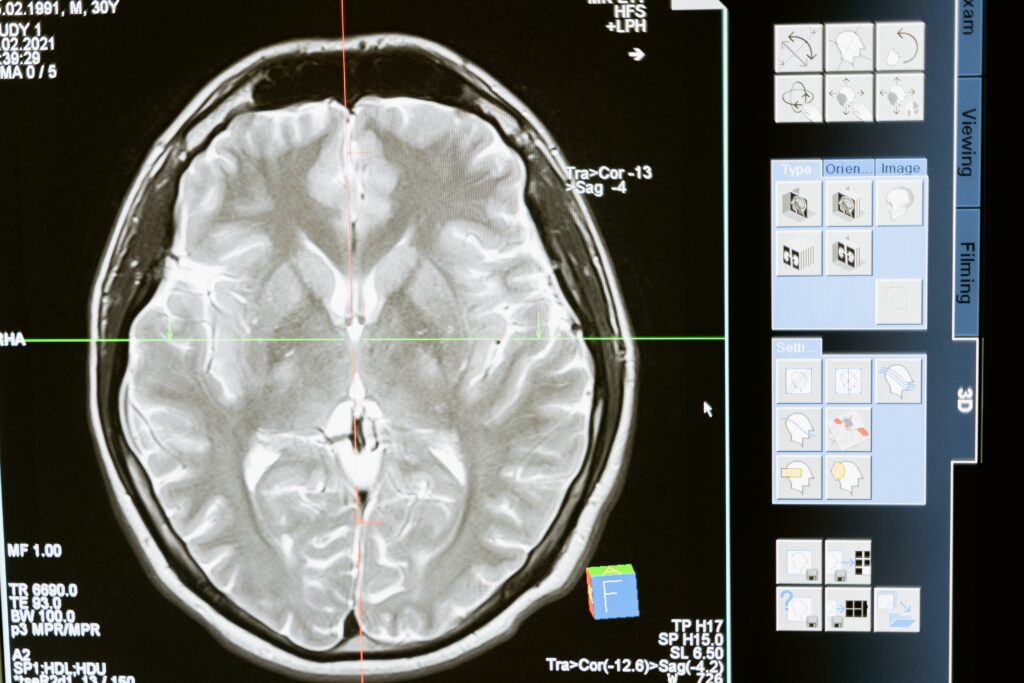
It’s clear, different countries do things differently, some incorporate brain scans into the process of determining if someone is brain dead, for example. As research evolves, guidelines may change, more can always be learned.

Responses